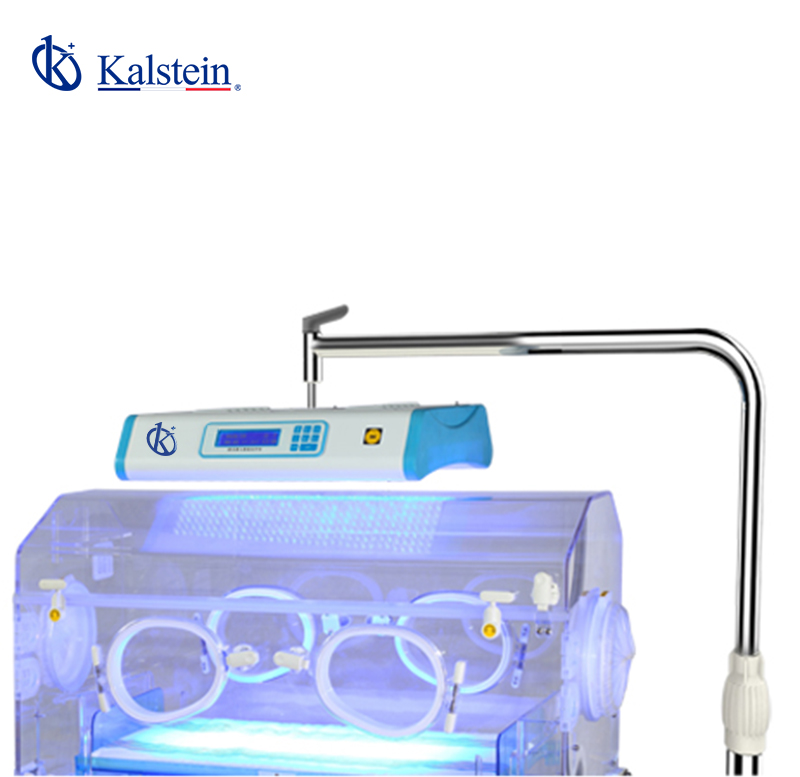
Phototherapy is a technique used in the neonatology unit to decrease bilirubin levels in the newborn. It is a simple technique consisting of placing a light at a distance of 30-40 cm from the naked body surface of the newborn after placing radiopaque glasses and removing any skin cream or lotion.
It is a therapeutic measure in the treatment of indirect hyperbilirubinemia, especially in those cases where the cause is not a severe hemolysis (incompatibility of RH or sub. Group). It consists of the therapeutic use of light and will be used even when other procedures such as exchange transfusion are used. It is also useful as prophylaxis of hyperbilirubinemia in preterm RN.
What is the purpose of the treatment?
The goal of treatment is to reduce the concentration of circulating bilirubin or prevent it from increasing. To do this, phototherapy uses light energy to modify the shape and structure of bilirubin, turning it into molecules that can be excreted even with poor normal conjugation.
The absorption of light by dermal and subcutaneous bilirubin leads to a fraction of the pigment experiencing several photochemical reactions at different levels. These reactions generate yellow stereoisomers of bilirubin and colorless derivatives of lower molecular weight. The products are less lipophilic than bilirubin and, unlike this, can be excreted in bile or urine without conjugation.
Types of phototherapy:
• Continuous, simple phototherapy: the phototherapy stays on 24 hours a day.
• Simple intermittent phototherapy: it consists of keeping the newborn for 4 hours with the phototherapy on and 4 hours with it turned off.
• Double or triple intensive phototherapy: it consists of introducing two or three phototherapies respectively.
Pathophysiology and treatment effect
Bilirubin is normally removed from the body by hepatic conjugation with glucuronic acid and elimination in bile in the form of bilirubin glucuronides. Neonatal jaundice derives from a temporary deficiency in conjugation (exacerbated in premature neonates), combined with an increase in red blood cell turnover. Pathological conditions that may increase bilirubin production include isoimmunization, hereditary hemolytic disorders and extravased blood (for example, from hematomas and cephalohematomas).
Genetic bilirubin conjugation disorders, especially the frequent Gilbert’s syndrome, can also contribute to neonatal hyperbilirubinemia. The largest group of usually healthy infants with the highest risk of hyperbilirubinemia are late preterm infants and those who are only breastfed (especially if breastfeeding difficulties occur). It is believed that breastfeeding and low caloric intake associated with breastfeeding difficulties increase enterohepatic bilirubin circulation.
Clinical use
In term and premature newborns, phototherapy is generally used according to the guidelines published by the American Academy of Pediatrics in 2004. 25 These guidelines take into account not only the level of total serum bilirubin, but also the gestational age of neonate, age in hours from birth and the presence or absence of risk factors, including isoimmune hemolytic disease, glucose-6- phosphate dehydrogenase deficiency, asphyxiation, lethargy, unstable temperature, sepsis, acidosis and hypoalbuminemia.
The effectiveness of phototherapy depends on the irradiation (energy) of the light source. Irradiation is measured with a radiometer or spectrometer in units of watts per square centimeter or in microwatts per square centimeter per nanometer within a given wavelength band.
Lamps with light predominantly within the blue region of the spectrum, between 460 and 490 nm, are probably the most effective for the treatment of hyperbilirubinemia. Currently, the American Academy of Pediatrics recommends special fluorescent blue lamps or proven light emitting diode (LED) lights.
In Kalstein we offer you a novel lamp for phototherapy highly applicable in hospitals and clinics, optimized for babies with jaundice. That’s why we invite you to take a look HERE